|
Excretion
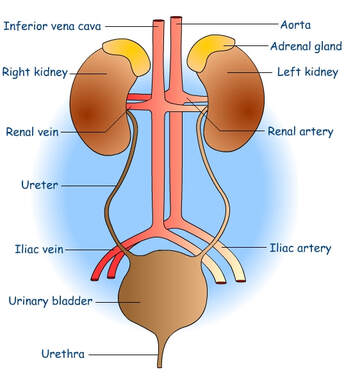
The process, by which waste product of metabolism from the system of an organism are eliminated from the body. Organs of the Excretory System
|
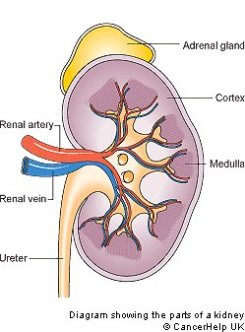
FUNCTIONS OF THE KIDNEYS:
- The kidneys remove urea and other toxic wastes from the blood, forming a dilute solution called urine in the process. The two kidneys have a very
- extensive blood supply and the whole blood supply passes through the kidneys every 5 minutes, ensuring that waste materials do not build up. The renal
- artery carries blood to the kidney, while the renal vein carries blood, now with far lower concentrations of urea and mineral ions, away from the kidney. The
- urine formed passes down the ureter to the bladder.
HOW DOES THE KIDNEY FILTER THE BLOOD:
Within each kidney there are an estimated one million microscopic nephrons, where blood filtration takes place. Each nephron contains a cluster of capillaries called a glomerulus. A cup-shaped sac called a Bowman's capsule surrounds each glomerulus. The blood that flows through the glomerulus is under great pressure. This causes water, glucose and urea to enter the bowmans capsule. White blood cells, red blood cells and proteins remain in the blood. As the blood continues in the excretory system, it passes through the renal tubule. During this time, reabsorption occurs: glucose and chemicals such as potassium, sodium, hydrogen, magnesium and calcium are reabsorbed into the blood. Almost all the water removed during filtration returns to the blood during the reabsorption phase. The kidneys control the amount of liquid in our bodies. Now only wastes are in the nephron. These wastes are called urine and include urea, water and inorganic salts. The cleansed blood goes into veins that carry the blood from the kidneys and back to the heart.
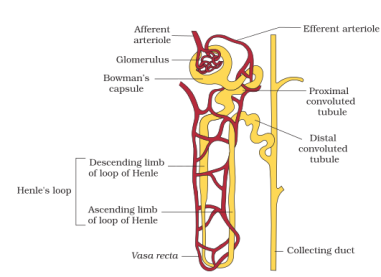
STRUCTURE OF A NEPHRON:
Within each kidney there are an estimated one million microscopic nephrons, where blood filtration takes place. Each nephron contains a cluster of capillaries called a glomerulus. A cup-shaped sac called a Bowman's capsule surrounds each glomerulus. The blood that flows through the glomerulus is under great pressure. This causes water, glucose and urea to enter the bowmans capsule. White blood cells, red blood cells and proteins remain in the blood. As the blood continues in the excretory system, it passes through the renal tubule. During this time, reabsorption occurs: glucose and chemicals such as potassium, sodium, hydrogen, magnesium and calcium are reabsorbed into the blood. Almost all the water removed during filtration returns to the blood during the reabsorption phase. The kidneys control the amount of liquid in our bodies. Now only wastes are in the nephron. These wastes are called urine and include urea, water and inorganic salts. The cleansed blood goes into veins that carry the blood from the kidneys and back to the heart.
STRUCTURE OF A NEPHRON:
|
|
<------TAKE A LOOK AT THIS VIDEO
|
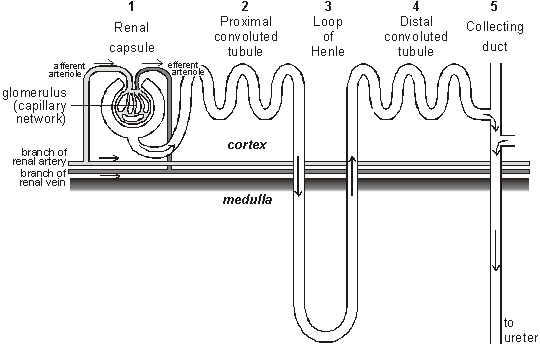
HOW DOES THE NEPHRON FILTER THE BLOOD:
STAGE 1: At the Renal capsule – Ultrafiltration occurs i.e. (FILTRATION UNDER PRESSURE)
The renal artery splits into numerous arterioles, each feeding a nephron. The arteriole splits into numerous capillaries, which form a knot called a glomerulus. The glomerulus is enclosed by the renal capsule (or Bowman’s capsule)- the first part of the nephron. The arteriole leading into the glomerulus (the afferent arteriole) is wider than the one leading out (the efferent arteriole), so there is high blood pressure in the capillaries of the glomerulus. This pressure forces plasma out of the blood by ultrafiltration. Both the capillary walls and the capsule walls are formed from a single layer of flattened cells with gaps between them, so that all molecules with a molecular mass of <70k are squeezed out of the blood to form a filtrate in the renal capsule. Only blood cells and large proteins remain in the blood.
STAGE 2: At the Proximal Convoluted Tubule – Reabsorption
The proximal convoluted tubule is the longest and widest part of the nephron. It is lined with epithelial cells containing microvilli and numerous mitochondria. In this part of the nephron over 80% of the filtrate is reabsorbed into the tissue fluid and then to the blood. This ensures that all
the “useful” materials that were filtered out of the blood (such as glucose and amino acids) are now returned to the blood.
*All glucose, all amino acids and 85% of mineral ions are reabsorbed by active transport from the filtrate to the tissue fluid. They then diffuse into the blood capillaries.
* Small proteins are reabsorbed and the amino acids diffuse into the blood.
* 80% of the water is reabsorbed to the blood by osmosis.
* Surprisingly, some urea is reabsorbed to the blood by diffusion. Urea is a small, uncharged molecule, so it can pass through membranes by lipid diffusion and there isn’t much the kidney can do about it. Since this is a passive process, urea diffuses down its concentration gradient until the concentrations of urea in the filtrate and blood are equal. So in each pass through the kidneys half the urea is removed from the blood and half remains in the blood.
STAGE 3: At the Loop of Henle - Water Reabsorption
The job of the loop of Henle is to make the tissue fluid in the medulla hypertonic compared to the filtrate in the nephron. The purpose of this “salt bath” is to reabsorb water as explained in Stage 5. The loop of Henle does this by pumping sodium and chloride ions out of the filtrate into the tissue fluid. The first part of the loop (the descending limb) is impermeable to ions, but some water leaves by osmosis. This makes the filtrate more concentrated as it descends.
The second part of the loop (the ascending limb) contains a Na+ and a Cl- pump, so these ions are actively transported out of the filtrate into the
surrounding tissue fluid. Water would follow by osmosis, but it can’t, because the ascending limb is impermeable to water. So the tissue fluid becomes more salty (hypertonic) and the filtrate becomes less salty (hypotonic). Since the filtrate is most concentrated at the base of the loop, the tissue fluid is also more concentrated at the base of the medulla, where it is three times more concentrated than seawater.
STAGE 4: Distal Convoluted tubule - Selective Reabsorption
In the distal convoluted tubule certain substances are actively transported from the blood into the filtrate, in other words they are secreted. It is relatively short and has a brush border (i.e. microvilli) with numerous membrane pumps for active transport. The important point about this secretion is that it is regulated by hormones, so this is the homeostatic part of the kidney. Substances secreted include H+ (for pH homeostasis), K+ (for salt homeostasis), ethanol, toxins, drugs and other “foreign” substances.
STAGE 5: COLLECTING DUCT - Urine Formation
As the collecting duct passes through the hypertonic salt bath in the medulla, water leaves the filtrate by osmosis, so concentrating the urine and conserving water. The water leaves through special water channels in the cell membrane called aquaporins. These aquaporin channels can be controlled by "Anti Diuretic Hormone" ADH, so allowing the amount of water in the urine to be controlled. More ADH opens the channels, so more water is conserved in the body, and more concentrated urine is produced. This is described in more detail in water homeostasis later.
The collecting ducts all join together in the pelvis of the kidney to form the ureter, which leads to the bladder. The filtrate, now called urine, is produced continually by each kidney and drips into the bladder for storage. The bladder is an expandable bag, and when it is full, stretch receptors in the elastic walls send impulses to the medulla, which causes the sphincter muscles to relax, causing urination
STAGE 1: At the Renal capsule – Ultrafiltration occurs i.e. (FILTRATION UNDER PRESSURE)
The renal artery splits into numerous arterioles, each feeding a nephron. The arteriole splits into numerous capillaries, which form a knot called a glomerulus. The glomerulus is enclosed by the renal capsule (or Bowman’s capsule)- the first part of the nephron. The arteriole leading into the glomerulus (the afferent arteriole) is wider than the one leading out (the efferent arteriole), so there is high blood pressure in the capillaries of the glomerulus. This pressure forces plasma out of the blood by ultrafiltration. Both the capillary walls and the capsule walls are formed from a single layer of flattened cells with gaps between them, so that all molecules with a molecular mass of <70k are squeezed out of the blood to form a filtrate in the renal capsule. Only blood cells and large proteins remain in the blood.
STAGE 2: At the Proximal Convoluted Tubule – Reabsorption
The proximal convoluted tubule is the longest and widest part of the nephron. It is lined with epithelial cells containing microvilli and numerous mitochondria. In this part of the nephron over 80% of the filtrate is reabsorbed into the tissue fluid and then to the blood. This ensures that all
the “useful” materials that were filtered out of the blood (such as glucose and amino acids) are now returned to the blood.
*All glucose, all amino acids and 85% of mineral ions are reabsorbed by active transport from the filtrate to the tissue fluid. They then diffuse into the blood capillaries.
* Small proteins are reabsorbed and the amino acids diffuse into the blood.
* 80% of the water is reabsorbed to the blood by osmosis.
* Surprisingly, some urea is reabsorbed to the blood by diffusion. Urea is a small, uncharged molecule, so it can pass through membranes by lipid diffusion and there isn’t much the kidney can do about it. Since this is a passive process, urea diffuses down its concentration gradient until the concentrations of urea in the filtrate and blood are equal. So in each pass through the kidneys half the urea is removed from the blood and half remains in the blood.
STAGE 3: At the Loop of Henle - Water Reabsorption
The job of the loop of Henle is to make the tissue fluid in the medulla hypertonic compared to the filtrate in the nephron. The purpose of this “salt bath” is to reabsorb water as explained in Stage 5. The loop of Henle does this by pumping sodium and chloride ions out of the filtrate into the tissue fluid. The first part of the loop (the descending limb) is impermeable to ions, but some water leaves by osmosis. This makes the filtrate more concentrated as it descends.
The second part of the loop (the ascending limb) contains a Na+ and a Cl- pump, so these ions are actively transported out of the filtrate into the
surrounding tissue fluid. Water would follow by osmosis, but it can’t, because the ascending limb is impermeable to water. So the tissue fluid becomes more salty (hypertonic) and the filtrate becomes less salty (hypotonic). Since the filtrate is most concentrated at the base of the loop, the tissue fluid is also more concentrated at the base of the medulla, where it is three times more concentrated than seawater.
STAGE 4: Distal Convoluted tubule - Selective Reabsorption
In the distal convoluted tubule certain substances are actively transported from the blood into the filtrate, in other words they are secreted. It is relatively short and has a brush border (i.e. microvilli) with numerous membrane pumps for active transport. The important point about this secretion is that it is regulated by hormones, so this is the homeostatic part of the kidney. Substances secreted include H+ (for pH homeostasis), K+ (for salt homeostasis), ethanol, toxins, drugs and other “foreign” substances.
STAGE 5: COLLECTING DUCT - Urine Formation
As the collecting duct passes through the hypertonic salt bath in the medulla, water leaves the filtrate by osmosis, so concentrating the urine and conserving water. The water leaves through special water channels in the cell membrane called aquaporins. These aquaporin channels can be controlled by "Anti Diuretic Hormone" ADH, so allowing the amount of water in the urine to be controlled. More ADH opens the channels, so more water is conserved in the body, and more concentrated urine is produced. This is described in more detail in water homeostasis later.
The collecting ducts all join together in the pelvis of the kidney to form the ureter, which leads to the bladder. The filtrate, now called urine, is produced continually by each kidney and drips into the bladder for storage. The bladder is an expandable bag, and when it is full, stretch receptors in the elastic walls send impulses to the medulla, which causes the sphincter muscles to relax, causing urination
HOMEOSTASIS - (SAME STATE)
Homeostasis describes the functions of your body which work to keep your internal environment constant within a very narrow range. One of your most important organs of homeostasis is the kidney.
Homeostasis describes the functions of your body which work to keep your internal environment constant within a very narrow range. One of your most important organs of homeostasis is the kidney.
|
|
<------TAKE A LOOK AT THIS VIDEO
|
ADH : Anti Diuretic Hormone controls the amount of water in the blood by controlling the amount of water excreted in the urine.
KIDNEY DISORDERS AND KIDNEY FAILURE :
|
|
<------TAKE A LOOK AT THIS VIDEO
|